Sick or Asthma? When Your Child’s Cough Won’t Go Away.
In May of 2015, Jack got a cough.
It just never went away.
Despite him acting totally normal, he would cough throughout the day, and it was especially bad at night.

Sometimes the coughing fits were so bad, it really scared me.
I felt like we were constantly going to the doctor – they would say come back if it doesn’t go away in 10 days (it never did). At that point, they’d go, “Well, maybe it’s allergies. We don’t like to call anything asthma at this age. Let’s give him azithromycin and see if that helps.” And it would…for a week or so, and the cough could come back.
And it would…for a week or so, and the cough could come back.
Finally, after several months of this and extensive allergy testing (that didn’t show any allergies), Jack was prescribed an inhaler.
No more coughing.
Oliver was recently diagnosed with asthma by his pulmonologist. He had been seeing a pulmonologist initially for his sleep apnea and GERD, but it was during one of his frequent visits that the doctor suggested that some of his symptoms pointed toward asthma.
We aren’t totally sure why they both have asthma – it could be genetics, the fact that they both had RSV as small infants increases their chances, and there are certainly environmental factors that play a part in it.
Regardless, it’s not the most fun diagnosis – especially because it often takes forever to get. Oliver’s pulmonologist said that the scenario I explained above is very common when a child goes into their pediatrician with a chronic cough.
Additional Reading: 5 Things to Consider When Your Child is Diagnosed with Asthma
So, does your child’s cough never go away?
It could be asthma. As Oliver’s pulmonologist says, there is no reason a healthy baby, child, or person should be coughing. If there’s a chronic cough, it should be looked into – especially if it happens during sleep.
A lot of pediatricians are hesitant to diagnose a child with asthma, and they will often call it “reactive airways disease.” Oliver’s doctor says this drives him crazy, because if it’s asthma, it should be called asthma. One of Jack’s old pediatricians would say that you couldn’t have asthma until you were five or older, which is not true.
As I mentioned above, it took awhile to get Jack’s diagnosis. We went through a lot of wasted time and sleepless nights waiting for his “cough” to blow over. So, my best advice to you parents out there who feel like your child’s cough will never end?
Be Proactive
It may not be asthma. There may be some other reason your child’s cough is not going away. However, you need to push for answers and for your physician to listen to you. No child should have to go through their childhood with a chronic cough!
One thing to know about asthma is that no one case is the same – there’s a very broad range of asthma severity and symptoms. Oliver’s pulmonologist often says that while wheezing is often associated with asthma, the lack of wheezing does not mean you don’t have asthma. Here are a few of the common symptoms of asthma, according to the Mayo Clinic:
- Frequent, intermittent coughing
- A whistling or wheezing sound when exhaling
- Shortness of breath
- Chest congestion or tightness
- Chest pain, particularly in younger children
- Trouble sleeping caused by shortness of breath, coughing or wheezing
- Bouts of coughing or wheezing that get worse with a respiratory infection, such as a cold or the flu
- Delayed recovery or bronchitis after a respiratory infection
- Trouble breathing that may limit play or exercise
- Fatigue, which can be caused by poor sleep
Find a Supportive Physician
I think having a supportive physician is crucial for just about any issues you or your child may have. We’ve discovered this a lot, especially with little Oliver. Once we found his pulmonologist, it made a world of difference. He encouraged us to ask questions from the start, and he spends as long as we need to with him (which makes up for the fact that we usually wait at least 30 minutes past our appointment time – we know he’s doing the same with others).
While most pediatricians are wonderful, they aren’t always specifically trained in treating asthma. If you suspect your child has asthma, I recommend seeing a specialist – typically a pediatric pulmonologist is your best bet. Asthma can be a very tricky thing to treat, and you definitely want the best on your side.
Identify and Eliminate Triggers
Asthma can be triggered by a lot of different things. For our boys, it seems like cold weather and illness is what triggers it the most (as well as smoke). What might be a simple cold in one child result in a very difficult few days of breathing for Jack and Oliver.
Even if your child hasn’t gotten an affiliate asthma diagnosis, I would pay attention to triggers to their cough. It can help control the symptoms as well as you can without formal treatment.
Many people who have asthma also deal with allergies – allergies to mold, dust, pollen, etc. There are a lot of them! On this Asthma Action Plan, it has a list of a lot of asthma triggers that you can go over. When we lived in our old house, we had neighbors that would always smoke at night. We had no air conditioning, and I was pregnant, so we left the windows open. However, we started noticing Jack’s coughing got worse. We couldn’t make our neighbors stop, and we couldn’t move, so we had to make adjustments.
What to Do When Your Child is Diagnosed with Asthma
Have an Asthma Action Plan
Once your child is officially diagnosed with Asthma, you will more than likely be given an asthma action plan. When we’ve been given one, it usually shows a green, yellow, and red zone (here is a pretty common template that is used).
It’s basically a plan that tells you when your child needs medication, when you should be worried, when you should increase dosage, etc. The goal is to always be in the green zone – which basically just requires a maintenance inhaler. This is a really important document to have on hand, as well as to share with anyone who may be watching your child.
The other day, Jack had one of his first real asthma attacks where we had to pull out his albuterol. We had used it when he was sick in the past, but this happened at the oddest time. He started wheezing like crazy. I was grateful that we knew what to do when that happened and were able to prevent anything worse from happening.
Be Consistent with Treatment
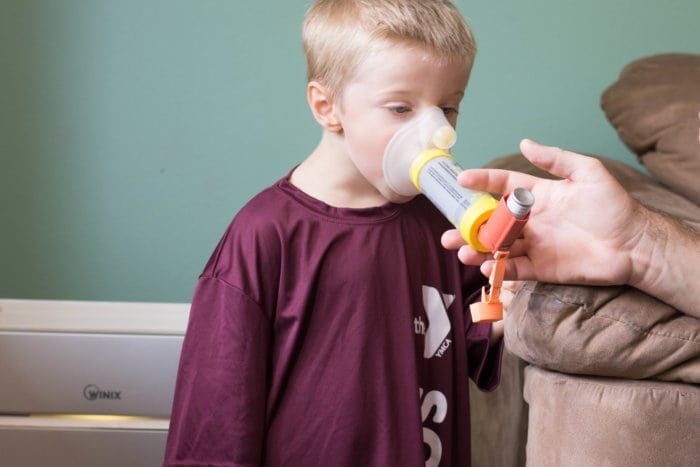
I’ll admit, I’m not the best at this. Jack usually gets his inhaler daily – he’s gotten to an age where he doesn’t fight it, and it is just a part of his routine.
Oliver is another story. There are few things I think he hates more than his inhaler, and it takes both Forrest and I to make sure he gets it. He screams like nothing else, and it is so, so sad. A few times we’ve tried to get him to do it after watching Jack – who he loves to copy – and it works for the first few puffs.
However, even if your child hates it like Oliver does, it’s so important to make sure you still give it to them. Prevention is the number one key to preventing asthma attacks and prolonged respiratory illness. As winter approaches, we are finding it even more important to keep up on their treatments.
Avoid Illness
Easier said than done – I know. I felt like with both of our boys, we do our very best to avoid sick people…but they just attract illnesses like no other children I’ve ever seen. It’s why I encourage people to keep their kids home f rom school, church, etc. whent hey are sick. You never know when you may have a child around who doesn’t respond well to illness.
Do the best you can and encourage healthy habits – teach your children to wash their hands regularly, use hand sanitizer when available, and honestly, don’t be afraid to tell sick people not to come over. Let me tell you, I’m all about sharing things…but germs is not one of them!
Find the Best Prices
Inhalers are expensive. If you are lucky, you will have an insurance plan that will significantly reduce the cost. However, if you don’t have great insurance (which, sadly, most people probably don’t), they are VERY expensive. It’s actually the reason why we can’t currently transfer our sons over to our health share plan – because the savings of that plan will be slashed by the cost of the inhalers.
There has been a lot of talk on the news sites about the increase in the cost of an EPI Pen…which I think is crazy (well, crazy that it was hiked up so much – not that it’s being talked about). However, it made me wonder why there isn’t more people pushing for lower priced inhalers. They can be life saving for people, yet the cost is so much.
Many doctors offices get samples, so ask your doctor if they have any available. They also often have coupons – you can check on websites like GoodRx.com to see if there are any printable coupons available, as well. Some inhalers are more cost-effective than others, so if you are finding you can’t afford the one your child uses, see if there is another more affordable one available.
Find Clean Air
We lived in Utah up until Jack was almost three-years-old. During the winter, the air is HORRIBLE. They often recommend that children and pregnant women don’t even go outside – and trust me, most people don’t want to. I believe that Jack’s issues were exacerbated because of the poor quality of air.
Despite family being in Colorado, one of the reasons we moved out of Utah is because we wanted to have cleaner air. Do I think it solved all our problems? Of course not. But I also think there’s a reason our boys get sick almost every time we drive into Utah Valley. If your child seriously struggles with asthma, look at where you live and avoid going out when the air is bad.
Another feature of the Winix that I love, is that the app tells you about the inside conditions AND the outside conditions. The light on the front indicates when the air quality in your home is supbar, and it also tracks the outdoor air quality. It tells you on the app how well the air purifier is working, as well as lets you know when you may need to replace the filters.

I love that it shows you how the air is in your house – if it starts to get iffy, you can rest assured it will be resolved soon, and until then, you can move to a different area. Being able to see the air conditions outside can help you decide whether or not it’s a good idea to let your child play outside much that day.








I like everything about his!! My oldest who is almost 5 could really benefit from this!! Wows at the price!!
My favorite feature is the filtration of 99.9 percent removal of bacteria out of the air, I live in Arizona and the dust is terrible and we all suffer from allergies in this dusty house!
I like that it tells you the inside conditions as well as the outside conditions.
This would be so awesome to have in our home!! I myself have asthma, and have suffered with it since I was diagnosed at around the age of 2. Our 2 daughters who are 6 and 3 have allergies as well. What I love about this is the App that tells things like the air quality inside and out, and that it tells when the filter needs to be changed! There really is an app for everything, isn’t there??
Thanks so much for the chance, and good luck to everyone!!
babydjs_mom@yahoo.com
I like the feature that can be quiet for the fan! Thanks so much for the chances to win.
I love that the coated Deodorization Carbon Filter combats offensive smoke, cooking and other household odors! Thanks for the chance!! ❤
Christymcmahon6@gmail.com
The coolest feature of this air purifier is how it is wifi! I also love the amazing filtration system that takes away 99.9% of bacteria in the air! I have a husband with asthma and a son with terrible allergies, so we could definitely use one of these.
We have a lot of allergies at our house. I take 2 allergy medications twice a day just on my own. Hubby takes meds twice a day due to food allergies and I have one child that takes allergy meds due to grass/pollen allergies (been to the ER ones with eyes swelled shut!). My favorite feature of this is that the carbon filter also works as a pre-filter to capture large particles such as hair, carpet fibers and dust adding life to your true HEPA filter. That’s so awesome!
I like this the most about their great product; a 5-Stage air purification system with Washable Pre-Filter, Coated Deodorization (CD) Carbon Filter, Anti-microbial True HEPA Filter
I love the set and forget option on there along with sleep mode!
The wifi is the coolest. Energy Star certified isn’t too shabby either.
I pretty much love everything about it. My lungs only function at 72% so there are a lot of things that make it hard for me to breathe maybe with this i would breathe better.
I pretty much love everything about it. My lungs only function at 72% so the little things really bother me and we have a bunch os animals so there is a lot of stuff in the air.
I love the fact that it has a Light Sensor that automatically puts unit on quiet fan speed and dims indicator lights once room lights are turned off.
Love the Wi Fi connectivity!
I love the sleep mode feature! My daughter has allergies and this would be great for her room at night and it would be quiet so it would be perfect!
I love the sleep mode and that it is wifi cool..
Wow…..this sounds like an awesome product. My favorite feature is the 4 speeds especially the “quiet” speed.
As someone that lives in an older home, I really need one of these. One thing that i found great about this product is it has an Anti-Microbial coated True HEPA filter captures 99.97% of airborne pollutants and allergens as small as 0.3 microns. Coating prevents bacteria and mold from growing.
I think the coolest feature of the Winix is the PlasmaWave technology that breaks apart pollutants at a molecular level without producing harmful ozone
Thank You for the great review and giveaway
I love that it’s wifi enabled!
The coolest feature is wifi. I cannot live without wifi.
I like the feature that the Winix HR1000 has WiFi enabled capability, and that I can get it right at The Home Depot.
I love the washable filters and this would help my wife so much who suffers from allergies badly
The light sensor feature is cool since it automatically put itself in a quiet mode, and the wi-fi feature is a plus to check the air quality indoors and out. We currently have different types of air filters in my kids room to help with their allergies and it is so easy to forget to check on them to make sure the filters are right and forget to turn off and on at the right times. The sensor and wifi will relieve my forgetfulness.
Anti-Microbial coated True HEPA filter captures 99.97% of airborne pollutants and allergens as small as 0.3 microns. Coating prevents bacteria and mold from growing — this is the most important for our family
Mt favorite feature is 5-Stage air purification system with Washable Pre-Filter, Coated Deodorization (CD) Carbon Filter, Anti-microbial True HEPA Filter and Winix PlasmaWave Technology
I love the Wifi technology. With having a daughter with allergies, especially during the dry winter heat, and a father in law that moved in with us after his stroke that has allergies, asthma, copd, and emphysema, this would be great to have in my house and be able to operate it through the Wifi. I also love that it has •PlasmaWave technology breaks apart pollutants at a molecular level without producing harmful ozone.
I love the Wi-Fi enabled- Ability to control unit via Winix Smart App and check air quality indoors and outdoors feature.
Aside from its Wi-Fi capabilities, I like that you have four different speeds; I’d be curious to see what the Turbo is like.
I like the sleep mode perfect for kids and family
The coolest feature of the Winix is the 5-Stage air purification system!
I love that it takes so much of the mold and pollens. I have asthma and there are times that it’s worse for me.
My favorite feature about the Winix HR1000 is that the Anti-Microbial coated True HEPA filter captures 99.97% of airborne pollutants and allergens as small as 0.3 microns. Coating prevents bacteria and mold from growing!!
I love that the Anti-Microbial coated True HEPA filter that captures 99.97% of airborne pollutants and allergens as small as 0.3 micron
I’m a geek, so I think the WiFi technology is really cool!! Plus also it just feels really relevant right now because my daughter has started waking up coughing every morning…..
i really like the light and sleep sensors!
I love so many of the features, that’s it hard to choose just one, but my favorite has to be the air quality sensor that provides a set-and-forget operation! That’s perfect for me!
Wi-Fi enabled- Ability to control unit via Winix Smart App and check air quality indoors and outdoors
I’m in Utah too! Sad how the air here gets so gross! I love the plasma technology feature, so it’s not harmful to the ozone.
I really like the light sensor feature. The air quality indicator is pretty cool too!
I love that it’s anti-microbial, really helps to clear everything!
I love that it has a Change Filter Alert! Sometimes I need a reminder like that!
The plasma wave technology sounds fantastic for breaking down particles erinnsluka@gmail
Oh this sounds so amazing and like it would help our family and little one so much! He has developed some of his daddies allergies, and can be so miserable at times. I think this would help our air so much, and also give me a great piece of mind that the air he is breathing is healthy clean air! I really love that the app tells you the quality of the air inside and outside your home. So amazing! Oh I think this sounds like a little miracle worker!
I love that it has a light sensor so you don’t have to readjust it when you go to bed!
Allergies are terrible this year.
I like that it offers the Air quality sensor providing set-and-forget operation. No more forgetting or having to re-set.
I Like the
Sleep mode , So it won’t interupt my sleep but it is still on..=)
I love that is has a air quality sensor. My husband and son have horrible allergies and this would help so much! Thanks so much for the chance.
Maybe it doesn’t qualify as cool but I love that it doesn’t put out ozone. I had a purifier that did and I’m convinced it made it more difficult for me to breathe.
I like that LED lights alert you to air quality changes and that I can control it from anywhere.
My husband has end stage COPD so stress about our indoor air quality quite a bit. I love that this machine monitors the air quality for me! Thank you for the chance to win!
Love how it can monitor indoors and outdoors air quality. Looks like a great product.
I think the actual app and wifi connection is an awesome perk of this model. Would be awesome to try !
When my son was little the doctor recommended that I get a air purifier for him and when it broke I did not get another because he seemed fine but in 2011 when he was 11 years old he got really sick he just kept coughing and I took him to the doctor 2 times in one week where they said to give him cough medicine and I sent him back to school where they called me and told me to pick him because he was coughing so much it was disturbing the whole class. I went straight from the school back to the doctor where they said they did’t know what was wrong with him and put him on antibiotic and a steroid. That night as my son slept I watched him and his chest was just caving in with every breath he took I rushed him to the hospital where is o2 was 89 they kept him for 2 days and said that it was a mix of asthma that was brought out with sickness and pneumonia. After we got out I got another one which as since quit working and this one looks awesome!! Thanks for the chance to win the feature I love the most about it is the coated carbon filter which takes out the smoke even from cooking and that it catches bigger objects such as hair which our dog loses alot of. This would be a great stress reliever.
Sorry so long.
I like that it has a washable filter. This would be a great product to clean the air in my home. Thanks for the info!
OMGoodness—I need this! Our allergies are brutal this year. I love the light sensor and sleep mode and the air quality sensor. This would be so easy to just set it and let it go.
I love that Light Sensor- Automatically puts unit on quiet fan speed and dims indicator lights once room lights are turned off
I like that it is Wi-Fi enabled.
I think the coolest feature is the Change Filter Alert.
I love that it is a 5-stage air purification system! The perfect was to get rid of pollutants, allergens, smoke, and household odors.
There is so much to like, especially that it captures 99.97% of airborne pollutants and allergens as small as 0.3 microns. We definitely need something like this in our home because of constant allergy and sinus problems.
I love the fact that it has a sleep mode where it puts the unit on quiet fan speed and dims indicator lights. It’s important to have quiet when I sleep. kristiedonelson(at)gmail(dot)com Thank you for this giveaway!
I like the air quality sensor. I have allergies triggered by dust and mold, so I bet this would help a lot.
Anti-Microbial coated True HEPA filter
I like that it has the ability to monitor indoor and outdoor quality! This would be so perfect for us. Thanks so much for the chance.
I absolutely love that it is Wifi compatible and also uses HEPA filters!
I like that this Winix has a washable pre-filter. That saves money!
I love that it informs you of the air quality both outside and inside. That would be very helpful for my husband and daughter.
I like that it’s wi fi enabled and has a sleep mode.
The coolest feature is being able to control it with an app, but I really like the Coated Deodorization (CD) Carbon Filter that catches carpet fiber, a real issue in our apartment.
The light sensor feature is really cool. I love that it is quieter once the room lights are dim.
I have asthma and so does my daughter. The feature that I like the best is that it has a washable filter. I dislike having to pay a lot of money for replaceable filters like I do on my water filtration systems.
I have a older house with pets. The washable air filters is a better option than the hpta filter on a regular air filter because have to replacing them.
I like the light sensor. My daughter suffers from allergies and asthma this would be perfect! With the light sensor it will not be to noisy or light
I like the light sensor that automatically puts the unit on quiet fan speed and dims indicator lights once the room lights are turned off…very cool!
I love the light sensor, energy cert and 4 fan speeds!
I love that it has 4 fan speeds. That is awesome. Anytime that there is a fan speed of quiet, I am sold! I have a dislike for loud noises. Ugh!
Best feature by far is the app that allows you to monitor both indoor and outdoor air quality. The more you know, the better decisions you can make for your family.
I LOVE that it tracks outdoor air quality too! I’ve never seen an air purifier that has so many neat options!
The app that tells you about the inside and outside conditions is a cool feature. You run these things and never really know how well they are working… this app takes care of that.
•Air quality sensor provides set-and-forget operation
This was the feature I liked the best but I also like the wifi feature.
the coolest feature of the Winix is that iThe carbon filter also works as a pre-filter to capture large particles such as hair, carpet fibers and dust adding life to your true HEPA filter
Air quality sensor provides set-and-forget operation Is the feature that grabbed my attention first.
The most amazing feature is that you can check the conditions of inside of your home and inside which would be wonderful for my family and I since we all have very bad allergies and asthma.
This would be perfect for your family!
I like this feature: Light Sensor- Automatically puts unit on quiet fan speed and dims indicator lights once room lights are turned off
The coolest feature for me is the Wi-Fi enabled- Ability to control unit via Winix Smart App and check air quality indoors and outdoors.
I love that it has a coating on the HEPA filter to prevent bacteria and mold from growing–the thought of mold in an air filter…yuck!
My daughter is almost 10. She was born with pneumonia and has struggled with asthma ever since. We work very hard to make sure her home environment is as safe as possible. My favorite feature of the Winix HR 1000 is the PlasmaWave Technology. I appreciate that it does not harm the ozone. I also like that it has Sleep Mode and Ligh Sensor capabilities which would be perfect for her at night. I appreciate the introduction to this brand….thank you!
the best feature is the Light Sensor- Automatically puts unit on quiet fan speed and dims indicator lights once room lights are turned off
Wi-Fi enabled- Ability to control unit via Winix Smart App and check air quality indoors and outdoors is cool cause you can check from any room great so i dont have to go in my kids room to check it
You are the winner! Please check your email for more details!
There are so many great features. My favorites are Wi-Fi enabled and the Sleep mode.
I think the coolest feature is the change filter alert because i always forget those things. Who has time to remember all the little things. This has alot of awesome features though I also really like that it has a quiet mode and that i can access it from my phone!
“True HEPA filter captures 99.97% of airborne pollutants and allergens as small as 0.3 microns.” – As someone who suffers from allergies all year round, this sounds fantastic.
I think the “sleep mode” feature is very useful. The sleep mode will run the fan at a quiet speed and dim all of the indicator lights. That is a unique feature.
It’s so important to me that an airfilter have the True HEPA filter so love that feature the most!
It may sound simple but my favorite feature that I read about is the light sensor. I know I personally am highly sensitive to lights at night. Driving is difficult, even small lights on electronics bother me at night, so to see that they sense when the light is off and dim to not be a disturbance is wonderful.
So wonderful that the air filter shows you the quality of the air inside and out!
I like the energy star feature and Air quality sensor provides set-and-forget operation
I love the sleep mode! It puts the fan on quiet and dims the lights on the machine!
I like the 4 Fan Speeds (Quiet, Medium, High, Turbo) feature. Perfect for night or day!
We have to use an Air Purifier because of my sons asthma. The one we have is no where close to being as nice as this one. I will have to look into upgrading mine now. The feature I liked the most is the Light Sensor. Bed time is always crazy and I always forget to turn down the purifier. This would come in handing at my house.
This would be an awesome win, as I have two little ones that suffer from asthma. First I’ve heard of this. Thanks for the info.
I like that it has a HEPA filter. I also learned that the carbon helps neutralize odors which I did not know. Seems like a great product.
The coolest feature is the Anti-Microbial coated True HEPA filter that captures 99.97% of airborne pollutants and allergens as small as 0.3 microns.
I like that it has a Coating that prevents bacteria and mold from growing. This has so many awesome features.
I love that it takes 99.97% of the yuck out of the air! we live in UT :/
I feel for you – Utah has the most horrible air!
Your poor boys! I had asthma growing up and it was no fun. I’m glad you guys have found ways to help make it better!