RSV in Babies: What All Parents Should Know

What is RSV?
If you’ve never heard the words “RSV” consider yourself lucky.
RSV is a respiratory illness our little family knows all too well. To some, it may seem just like a common cold.
That’s how it presents itself in most people.
Unless, of course, it’s a baby. Then it’s a whole other story.
That cold that just was an inconvenience to you? Well, this is what can happen when a baby picks it up:
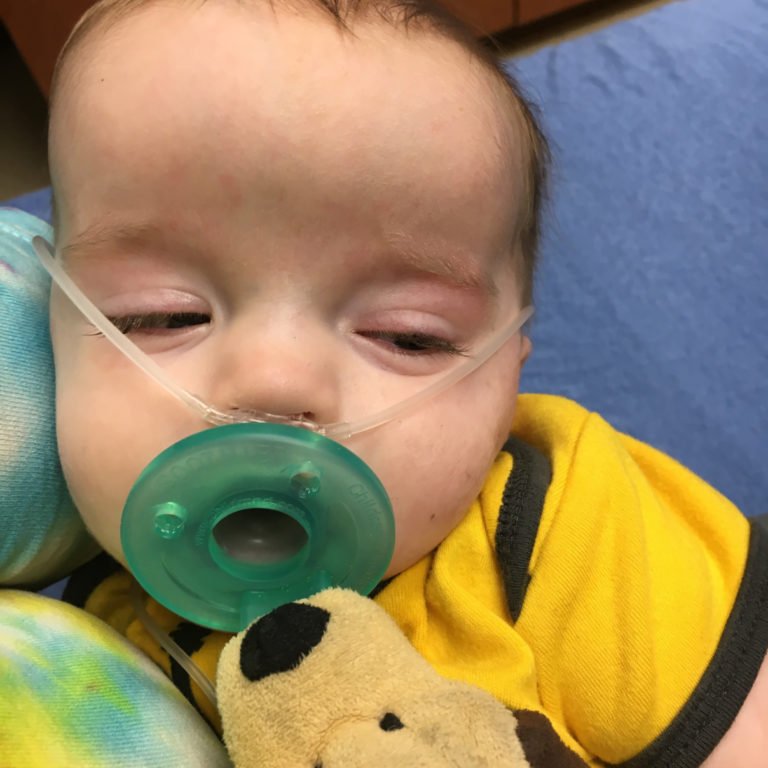
and this:
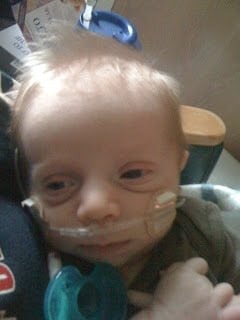
Those are both of my boys – both of which got RSV. Jack got it when he was two weeks old, Oliver five months.
No parent should be told there are dead people with higher oxygen levels than their two-week-old baby.
One of my biggest fears with Oliver was that he would get it, and that fear came true just a few weeks ago.
RSV is nasty. And it’s scary. And it’s something all new parents need to know about.
I had no idea what it was until Jack was admitted to the hospital with it, and it’s something I wish I didn’t know anything about! But I do, and after seeing first hand (two times) how scary it can be in a tiny little baby, I want to share that with others.
So, new parents, listen up.
Here’s what you need to know about RSV.
RSV (respiratory synctial virus) respiratory virus that is extremely contagious. It’s also very common and most children have it before the age of two.
While it may just appear as “the common cold” in many children, it’s also one of the most common reasons for hospitalizations of babies.
And you never know how your baby will react to it. They might just get the sniffles, or they may end up in the hospital like my boys.
The number one way to prevent it is to keep your child away from sick people. It gets harder when you have other kids who you can’t exactly keep cooped up all winter long. But the more you can keep your baby away from sick people the better.
Don’t be afraid to turn people away or to question if they’ve been sick lately.
And if you’ve been sick? Stay home. The best gift you can give a family with a new baby is to keep your germs to yourself.
Keep hand sanitizer around and make sure you (and your other kids) wash your hands vigilantly.
Heck, you may even want to keep some disposable face masks around the house, just in case someone does get sick (that you can’t banish from the house!
RSV Prevention
There is a vaccine for RSV but it is only available for preemies. Beyond that, prevention just comes down to washing hands regularly and staying away from sick people!
Complications of RSV
Most babies will recover just fine from RSV - it just hangs on FOREVER! When Jack had it, the doctors warned us that he would likely be more prone to respiratory problems in the future, which we've found to be true. He gets sick really easily, and he has also developed asthma.
(Update: Oliver was recently diagnosed with asthma as well, and his doctor believes it's because of his early exposure to respiratory illness).
Listen to your instincts. If you think something is wrong with your baby, go with your gut.
With both my boys, I knew something was wrong, and I sought a second opinion. BOTH times we had been seen earlier in the day by another doctor who dismissed our concerns.
I can't even think about what would have happened had I not listened to my instincts, seeing the shape he was in when he arrived at the hospital.
You know your baby better than anyone.
And when it comes to a baby, I don't think you can ever be too careful.
Originally written in 2016; updated in 2019







This is my first time experiencing rsv. It is so scary. I just had my fifth child two wks ago today and we found out him and my fifteenth month old has RSV. My newbie Apollo had to be hospitalized because they didn’t wanna take a chance even tho at the time his oxygen level was 99 and he was sounding good. We’ve been in this hospital since Monday morning and we were gonna be sent home today but the doc wanted to make sure Apollo could be taken off the oxygen while sleep and it not drop from 90’s to 80’s. He did ok today better than yesterday but it still wasn’t where they wanted it to be. Their main concern is it being low while he’s asleep. Reading ur story actually soothed and educated me. I am so scared for Apollo I just don’t want it to turn into anything else. My fifteenth month old Akylez is doing good. He is older so it’s not as bad on him thank God. I pray everything works out for my boys. Thanks for sharing your story.
I’m so sorry that you went through this. I hope your children have recovered okay!
Hello my son was born on 10/26 and we’re currently in the hospital because he has RSV. We came in on November 17th 2018 and currently still here. They’ve had him on oxygen but currently took him off to see how he does. His level are at 89 and 90 but they say he’s starting to look good if we want to try to go home we can. I told them will stay another day to monitor it to make sure he does good. This post was very informational thank you. Also what were your boys levels when y’all went home? My son is eating and pooping and peeing well. I’m just worried because his cough is still really ugly?
Oh my! That sounds so hard. I’m so sorry. Both of my son’s came home on oxygen because their sats were dropping to the low 80s/high 70s still. Jack was on oxygen for about two weeks, Oliver was for about a week.
So sorry to hear that but glad they’re doing better. I’m just so nervous about going home he does sound much better I’m just terrified. He is my 5th child but first time going through this.
Whether it’s your first or fifth, it’s so scary to have a little one in the hospital. It will be okay! Definitely don’t let them send you home until you feel ready <3
Great post! I was a peds nurse on a respiratory floor for three years and RSV (and flu) season are no joke. We sometimes had to send kids to the ICU for being so sick from it. Even older kids can have complications, especially if they’re asthmatic or have other pulmonary issues.
Hopefully someone will be able to make a similar drug to Synagis soon so it will be widely available. The patents are expired but it’s apparently a lot of work to produce something similar. We can only hope!
Thanks for commenting! I hope they’ll be able to make a drug like that available for all soon! Such a scary illness.
My son Elliott(4months old) was diagnosed with pneumonia on Feb. 28th, then the very next day in the evening I noticed he was sucking in at the bottom of his ribs and using his belly to help him breathe, his nose was flaring and he seemed to start to struggle more. So I went with my gut and rushed him to the local ER. They did a swab for influenzas, and RSV. The test came back negative for influenza and positive for RSV. My heart raced and I began to google and I freaked out and put the phone away. They sent him home with a nebulizer. The albuterol seems to help him a lot. He does tend to get a little agitated but not too bad. His oxygen has been in the 90’s and he is staying hydrated and plenty of wet diapers. So I hope and pray he stays on this path to healing and out of the hospital. 90% of the time we stay home, my kiddos are kept away from brother when they are sick, but my youngest daughter had a cold a week ago, this time she wasn’t listening to mommy about staying away from brother. So I’m sure that’s probably where he got it. ? He has been through so much already it breaks my heart to see him go through another thing.
Bailey was born Nov 11 2017 and passed away Jan 25 2018.
I’m so sorry.
My son was admitted with RSV at 18mos old, he also has Down Syndrome. He was in the hospital for 2 wks and had gotten double pneumonia before recovering. He developed asthma from it which plagued him for about 6 years before it dissipated. He rarely needs any breathing treatments now unless he has a severe respiratory infection. His diagnosis and hospitalization was very scary. We also had been told by a physician to take him home, he was cyanotic–which the Dr. disagreed with, lethargic and non responsive. Yet we were told to bring him home. I urged her to take a oxygen test on him and when it read out at 78 I was told to go immediately to the hospital without packing first. He nearly died. I wouldn’t allow her to treat him ever again, she treated him initially b/c my son’s Dr. was not in. I found out later from my sitter that her son was ill with a respiratory infection and she put my son in the crib with her son, that is most likely how my son got RSV. Needless to say I changed sitters. Thank you for telling your story, it was quite informative about a common illness that we are not normally educated about.
The sad thing about this is the vaccine should be available to all kids. Insurance companies only give it to babies because it’s so expensive and they don’t want to pay for it. We ended up paying $4282 per shot for it because our child is on oxygen and high risk (we have a really high deductible). She has to get it every month during the winter so that is 3-4 shots (one per month). How sad insurances and money grubby companies dictate our children getting REALLY sick.
Sorry I meant they only give it to preemies… it should be available to all babies and children!
I completely agree – all children should have it accessible to them. It’s unfortunate because RSV is SO contagious and such a serious illness. I’m sorry to hear about your daughter – it just doesn’t seem right that someone has to spend so much just to keep their child well. Oliver just started coughing and having a runny nose tonight, and it makes me so nervous (apparently RSV is really bad this year in Denver). I hope your little one stays well!
That response was from Katie, not Forrest 🙂
This is such a great post. We really do need to spread the word so people can know more and come in before it’s too late! I’m so sorry you’ve had to go through it TWICE! Hopefully you won’t ever have to face it again! And you definitely know the warning signs now!
I am hoping that sharing my story can help someone else!